
Healthcare costs are rising — here’s what that means for your benefits and your wallet (and three simple steps to act)
States with health insurers requesting highest premium rate change (2026)
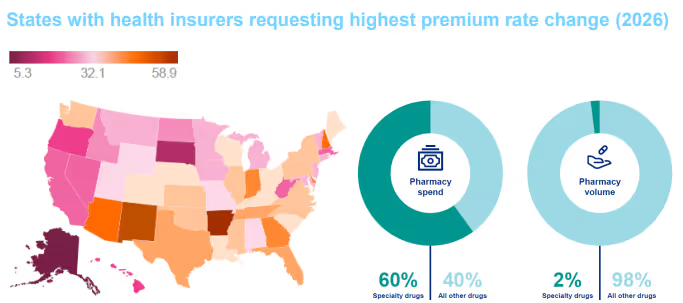
Much of the increase is coming from specialty medicines (especially oncology drugs) and the rapid rise of GLP-1 drugs used for weight loss and diabetes. These drugs are expensive, often ongoing, and are shifting pharmacy spending dynamics (Marsh & McLennan Agency; RAND analysis on GLP-1 use) (https://www.rand.org/pubs/research_reports/RRA4153-1.html).
Pharmacy cost trends were 2.5 points higher than medical cost trends in 2025. The specialty pharma market grew from $92.5 billion in 2023 to $129.23 billion in 2024. It is expected to reach $965.5 billion by 2030.
Average annual change in prescription drug benefit cost per employee (after rebates), among employers with 500 or more employees
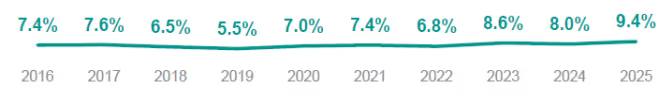
Expect higher costs — but there are handles to manage them
Health spending is up across medical and pharmacy lines; specialty drugs account for a large share of pharmacy dollars even though they’re a small share of prescriptions.
Annual changes in health benefit costs, workers’ earnings, inflation, and market trends (2010–2025)
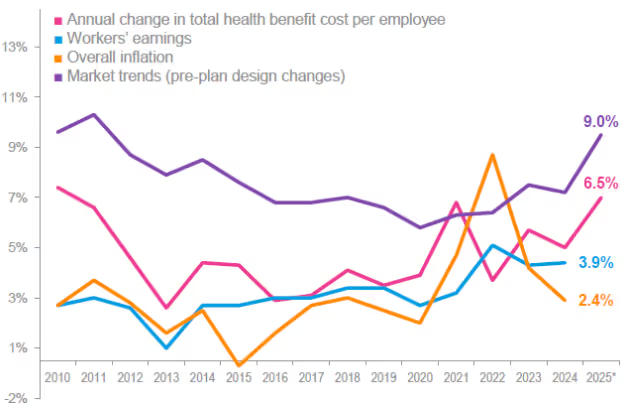
Action: Ask your broker/benefits team about targeted cost levers (specialty drug strategies, site-of-care steering, stop-loss design).
Pharmacy (and GLP-1s) will be front-and-center
GLP-1s and other specialty therapies are major cost drivers; usage has surged. Employers are tightening access and adding prior authorization, lifestyle requirements, or outcomes-based contracting to manage use and cost.
GLP-1 medications are rapidly changing how conditions are managed. Originally prescribed for diabetes, they are now used to treat a wide variety of conditions, both off-label and with FDA approval.
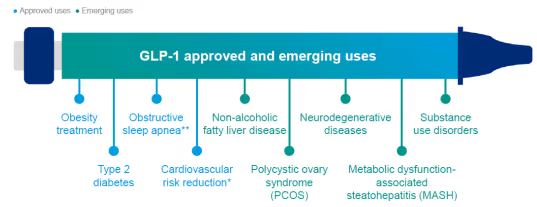
11.8% of U.S. adults used a GLP-1 medication in 2025 to lose weight or treat chronic conditions like diabetes or heart disease, while 14% reported interest in starting treatment.
Action: Review PBM contracts, require transparent pass-through pricing, consider biosimilar-first approaches and step therapy where clinically appropriate.
Use data and transparency to negotiate better deals
New federal transparency emphasis offers more pricing data for plan sponsors to negotiate smarter networks and steer members to lower-cost, high-quality providers (White House price-transparency
order: https://www.whitehouse.gov/presidential-actions/2025/02/making-america-healthy-again-by-empoweringpatients-with-clear-accurate-and-actionable-healthcare-pricing-information/).
Action: Ask your broker for network benchmarking and clarity on how transparency data was adjusted/validated before you make plan changes.
Quick, practical next steps for clients (what producers should recommend)
Review pharmacy contracts now (PBM transparency, biosimilar strategy, prior authorization rules).
Re-run renewals with scenario modeling that includes GLP-1 uptake and specialty oncology cases.
Audit plan communications to reflect OBBBA changes (HSA/DPC/FSA/Trump Accounts) and upcoming state mandates (e.g., fertility/IVF mandates). (OBBBA text: https://www.congress.gov/bill/119th-congress/housebill/1/text/pl).
Expand navigation, mental fitness coaching, and eldercare supports — high perceived value, often lower cost.
Insist on AI governance and training before rolling out employee-facing tools
Works Cited
EHB 2026 Trends Presentation — Marsh & McLennan Agency LLC
2026 Employee Benefits Market Outlook — Zywave / Marsh McLennan Agency
5 Employee Benefits Trends Shaping 2026.pdf — Zywave
2026 EHB Trends Placemat.PDF — Marsh & McLennan Agency LLC








.png)




.png)

.avif)


